It can be dangerous to delay a cavity filling, but not usually in the dramatic way people imagine. The real risk is that a cavity tends to grow. If it spreads deeper, a simple filling may no longer be enough, and you may need more complex care, such as a root canal, a crown, or even tooth removal. The earlier you treat a true cavity, the easier it usually is to fix.
If you have swelling, fever, pus, or rapidly worsening pain, that can signal infection, and you should be seen urgently.
Table of Contents
If you delay a cavity filling, here is what commonly happens
- The cavity usually gets bigger, which means more tooth has to be removed later.
- Symptoms can start or change (cold sensitivity, sweet sensitivity, pain with biting).
- The tooth can weaken, increasing the chance of chipping or cracking, especially on back teeth.
- The nerve can become inflamed or infected, which may require a root canal rather than a filling.
- In some cases, an abscess develops, and that is where it can become urgent (swelling, fever, pus, feeling unwell).
An important nuance
Very early “starting” areas of decay (non-cavitated lesions) can sometimes be managed with fluoride and monitoring instead of drilling right away, depending on your risk level and what the dentist sees on exam and X-rays.
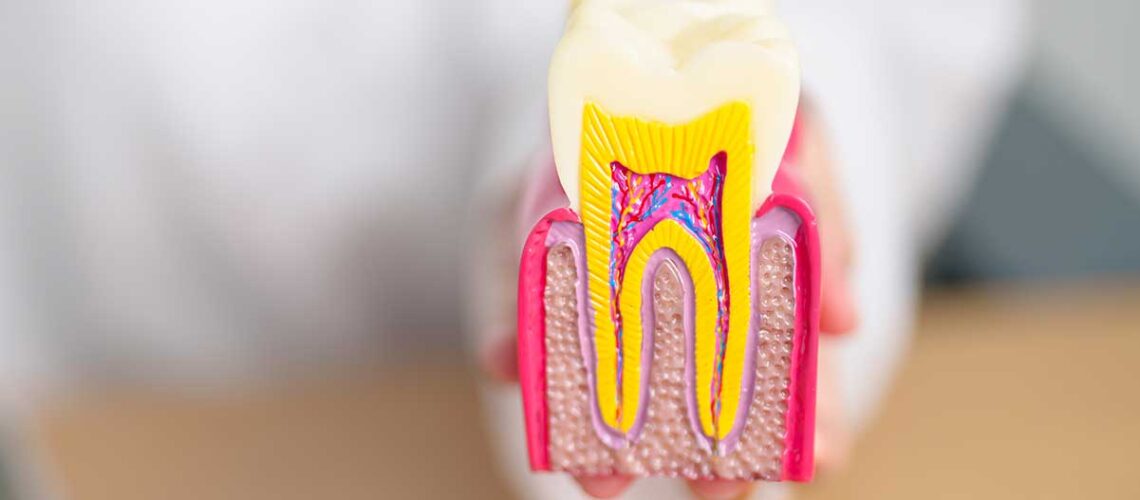
Why delaying matters: how a cavity progresses inside a tooth
Think of a tooth like layers:
- Enamel: the hard outer shell
- Dentin: the softer inner layer under enamel
- Pulp: the nerve and blood supply in the centre
Early stage: demineralization (sometimes reversible)
In the earliest stage, minerals leach out of enamel. This can look like a chalky white spot. If there is no actual hole, and if your risk is low, dentists may recommend fluoride and monitoring because remineralization can be possible.
Once there is a hole, bacteria have a shelter
Once enamel breaks down into a cavity you can catch with an instrument or see as a true defect, plaque and bacteria can hide where a toothbrush cannot reach well. At that point, the area often keeps progressing unless it is restored.
Dentin stage: things can speed up
Dentin is softer than enamel, so once decay reaches dentin, cavities often progress faster. This is also when people begin to notice sensitivity to cold, sweets, or a quick zing.
Pulp stage: inflammation, then infection
If bacteria reach the pulp, the nerve can become inflamed. Sometimes that starts as short, sharp pain. If it progresses, pain can linger, wake you up, or make chewing painful. Eventually infection can develop, which may require root canal treatment to save the tooth.
Abscess: where “danger” becomes more real
A dental abscess is a pocket of pus caused by infection, and it needs prompt dental care. It can cause swelling, fever, and feeling unwell.
“My cavity does not hurt.” Does that mean it is safe to wait?
Not necessarily.
Pain is helpful information, but it is not a perfect early warning system. Some cavities are painless because:
- the decay is still in enamel or early dentin
- the cavity is growing in a direction you do not feel yet
- the tooth nerve is not irritated until later
- your bite and chewing patterns avoid the spot
That is why dentists rely on X-rays and clinical signs, not only symptoms, to judge depth and urgency.
Also, patients commonly describe a spot as “tacky” or “sticky,” or say food keeps getting stuck. That can be a real clue that bacteria are getting a protected home.
When waiting might be reasonable (and when it usually is not)
Getting a cavity filled can often be a bit of a hassle in terms of time and money, and even if your dentist makes it a comfortable experience, it still won’t be fun. That’s why it might be tempting to ask if a cavity even needs to be filled (at least not right away).
Situations where monitoring can be appropriate
Your dentist might recommend a watch and monitor approach when:
- the area looks like early, non cavitated decay
- it is confined to enamel or shallow and not clearly cavitated on exam
- you are low risk for cavities and have good fluoride exposure
- the dentist can re check it with X rays or photos and you can follow prevention steps
This conservative approach lines up with modern caries management: assess risk, treat early lesions non-surgically when possible, and restore when cavitation is present.
Situations where delaying is more likely to backfire
Delaying becomes riskier when:
- the cavity is cavitated (a real hole)
- it is into dentin on X ray
- you are high risk (frequent cavities, dry mouth, lots of snacking, poor fluoride exposure)
- the tooth already has a large filling or crack lines
- you have symptoms that are trending worse
Signs your cavity may be getting worse
A cavity can worsen quietly, especially early on, so the first clues are often small changes like sensitivity, food trapping, or a tooth that starts to feel different when you bite.
- cold sensitivity that is new or increasing
- sensitivity to sweets or acidic drinks
- pain when biting or chewing
- a dark spot that seems to spread
- a rough edge, chip, or food trapping
- a bad taste that keeps returning
Red flags that should be treated as urgent
Seek urgent dental care (same-day if possible) if you have any of the symptoms below, especially if they are worsening, spreading, or you feel unwell, as these may indicate an infection or abscess.
- facial or gum swelling
- fever, chills, or feeling unwell
- pus or a pimple-like bump on the gums
- trouble swallowing, or difficulty opening fully
- severe pain that is not controlled
What to expect at the appointment
A filling appointment is usually straightforward, and knowing the steps ahead of time can make it feel a lot more predictable and manageable.
Step 1: confirm what is actually happening
- reviewing symptoms (including “none”)
- checking the tooth, gums, and bite
- X-rays if needed, to see between teeth and depth
- a simple plan: fill now, monitor, or treat more deeply if needed
Step 2: the filling itself (the usual flow)
While every clinic differs, a typical filling visit includes:
- numbing (freezing)
- isolating the tooth
- removing the softened decayed tooth structure
- placing and shaping the filling material
- checking your bite and polishing
Step 3: normal after effects
It can be normal to have:
- mild sensitivity for a short period
- a “high spot” feeling if the bite needs adjustment
If pain is severe, worsening, or lingering, you should call the office because it can sometimes mean the filling is close to the nerve, the bite is high, or another issue needs attention.
Why “a simple filling” can turn into bigger treatment if you wait
Bigger cavity means bigger restoration
As decay spreads, more tooth needs to be removed to clean it out. Larger fillings have less natural tooth supporting them, and some teeth then need an indirect restoration (like an onlay or crown) for strength.
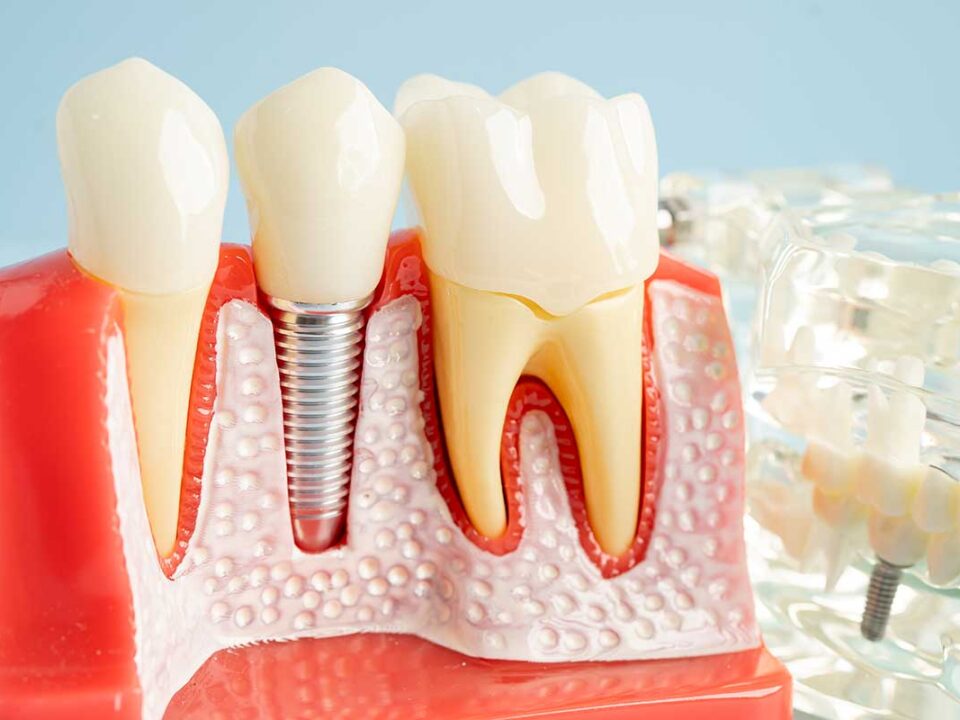
Once the nerve is involved, the goal changes
A filling repairs tooth structure. A root canal treats infected or inflamed pulp tissue inside the tooth. When decay reaches the pulp, a root canal may be needed to keep the tooth.
Infection can spread beyond the tooth
This is less common, but it is the reason dentists take abscess symptoms seriously. Health systems describe dental abscesses as requiring urgent treatment and not resolving on their own.
“Can I heal a cavity at home?”
This is one of the biggest myths online, so no, you can’t heal an actual cavity.
What is sometimes possible
Early enamel demineralisation may be arrested or remineralised with fluoride, diet changes, and better plaque control, especially when there is not a true hole yet.
What is not realistic
Once there is a cavity you can catch or a hole, brushing cannot rebuild missing tooth structure. You may slow it down, but you usually cannot reverse a cavitated defect without professional care.
Practical prevention while you are waiting for your visit (safe, general guidance)
This is not a substitute for diagnosis, but these habits can reduce risk:
- brush twice daily with fluoride toothpaste
- clean between teeth daily (floss or interdental brushes)
- reduce frequent sipping and snacking on sugary or acidic items
- drink water regularly, especially if you have dry mouth
- keep regular checkups so early changes are caught sooner
If you are anxious or embarrassed about delaying
You are not alone. A lot of people delay dental care because of fear, financial stress, past experiences, or busy lives. Online, people openly talk about dental anxiety, embarrassment, and feeling “traumatized” by past care, which can lead to avoidance.
What I tell patients is that we would rather see you now than later, and our job is to help you move forward without judgment. If you are nervous, say it at the start of the visit. It helps the team adjust pacing, explain more, and keep you comfortable.
Frequently Asked Questions (FAQ)
There is no universal safe timeline because cavity speed depends on the tooth, the location, and your risk factors. In general, once a dentist confirms a cavitated lesion or dentin involvement, earlier treatment usually lowers the chance of needing bigger procedures later.
It can be both. Many delays start as “just uncomfortable,” but the danger comes if the decay reaches the pulp or an infection develops. Abscess symptoms are the main reason a delay can become urgent.
Early decay can be limited to enamel or shallow dentin, and the nerve may not be irritated yet. Also, the cavity may be in an area that does not get pressure when you chew. That is why X rays and exam findings matter.
Yes, it can. If decay reaches the pulp and causes irreversible inflammation or infection, root canal treatment may be recommended to save the tooth.
Warning signs include lingering heat pain, spontaneous throbbing, pain that wakes you up, swelling, or a gum boil. Your dentist will confirm with tests and X rays.
Not automatically. Watching can be appropriate for early, non cavitated lesions, especially when you are low risk and the dentist has a plan to monitor changes over time.
The bacteria involved in cavities can be shared (for example through saliva), but cavity development depends on diet, oral hygiene, fluoride, and individual risk factors. It is more accurate to think of cavities as a disease process rather than a simple infection you “catch.”
Usually not. But it is still time sensitive because “small” can become “bigger” without obvious symptoms. It becomes urgent if you have swelling, fever, pus, or severe pain.
The decay itself is local to a tooth surface, but the habits and conditions that cause cavities can affect multiple teeth. Also, food trapping areas and plaque retention can increase risk for neighbouring surfaces.
In many cases, yes, dental care is encouraged during pregnancy, and treating active decay can prevent future infection. Timing and materials can be discussed with your dentist and obstetric provider for your specific situation.
Not always, but bitewing X rays are commonly used to detect cavities between teeth and estimate depth, especially when the tooth looks fine on the surface.
Book the next available visit and ask to be placed on a cancellation list. Meanwhile, keep fluoride brushing consistent and reduce frequent sugar exposure. If symptoms escalate, call back.
Dentists usually use local anaesthetic (freezing) so you should not feel sharp pain, though you may feel pressure. If you feel pain, tell the team so they can adjust anaesthetic.
References
- Canadian Dental Association. (n.d.). Cavities. Accessed February 24, 2026.
https://www.cda-adc.ca/en/oral_health/talk/complications/diseases/cavities.asp - Canadian Dental Association. (n.d.). Fillings. Accessed February 24, 2026.
https://www.cda-adc.ca/en/oral_health/procedures/fillings/index.asp - Ontario Dental Association. (n.d.). Cavities and tooth decay. Accessed February 24, 2026.
https://www.oda.ca/oral-health-basics/oral-conditions-diseases/cavities-tooth-decay/ - NHS. (2025, August 13). Tooth decay.
https://www.nhs.uk/conditions/tooth-decay/ - NHS. (2022, June 20). Dental abscess.
https://www.nhs.uk/conditions/dental-abscess/ - National Institute of Dental and Craniofacial Research. (2025, September). Tooth decay.
https://www.nidcr.nih.gov/health-info/tooth-decay - Mayo Clinic Staff. (2023, November 30). Cavities and tooth decay: Symptoms and causes.
https://www.mayoclinic.org/diseases-conditions/cavities/symptoms-causes/syc-20352892 - Mayo Clinic Staff. (2022, June 29). Tooth abscess: Diagnosis and treatment.
https://www.mayoclinic.org/diseases-conditions/tooth-abscess/diagnosis-treatment/drc-20350907 - American Dental Association. (2023, July 18). Caries risk assessment and management.
https://www.ada.org/resources/ada-library/oral-health-topics/caries-risk-assessment-and-management - Moreau, A. M., Dumais Pelletier, S. È., Nguyen Ngoc, C., Rompré, P. H., & Vu, D. D. (2022, March 8). Clinical management of interproximal and occlusal caries in children and adolescents by Canadian dentists: A survey. Journal of the Canadian Dental Association, 88, m3.
https://jcda.ca/m3 - American Association of Endodontists. (n.d.). Root canal explained. Accessed February 24, 2026.
https://www.aae.org/patients/root-canal-treatment/what-is-a-root-canal/root-canal-explained/ - International Caries Classification and Management System. (n.d.). ICCMS Quick Reference Guide for Practitioners and Educators (PDF). Accessed February 24, 2026.
https://www.iccms-web.com/uploads/asset/5928404ea4df6343406124.pdf
Check us out on Facebook and Twitter for daily information about Oral Health from Martindale Dental, or visit our offices in Hamilton and St. Catharines.
Have more questions?
Please contact us for all inquiries or to book an appointment with one of our convenient clinic locations. We look forward to hearing from you.