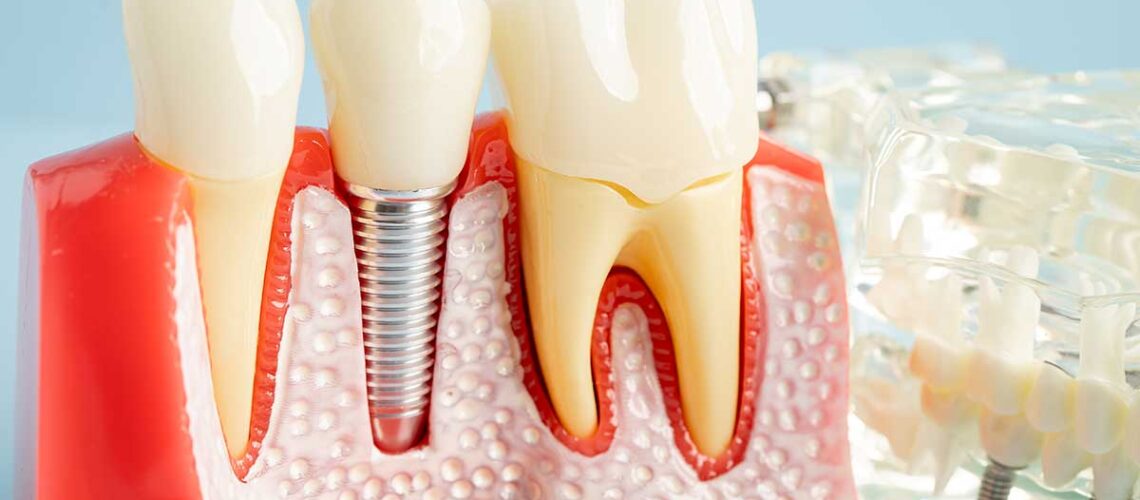
If you have a dental implant and you are noticing bleeding, swelling, tenderness, or a weird taste, it is totally normal to wonder, “Is this just irritated gums or is my implant infected?” Peri implantitis is essentially gum disease around an implant, and the key difference is that it involves inflammation plus progressive bone loss over time. The good news is that catching issues early often gives you more options.
Table of Contents
The direct answer: What are the signs and symptoms of peri-implantitis (implant gum disease)
Peri-implantitis is inflammation around a dental implant with progressive bone loss. Your dentist confirms it with a combination of clinical findings and X-rays, but the warning signs people notice at home are often pretty consistent. If you are searching “infected dental implant signs,” “implant gum bleeding,” or “bad taste around implant,” this is the exact checklist we talk through in clinic.
Common signs and symptoms of peri-implantitis include:
- Bleeding around the implant when brushing, flossing, or using a water flosser
- Red, puffy, or swollen gum tissue around the implant crown
- Pus or discharge, or a bad taste that keeps returning
- Deepening gum pockets around the implant (your dentist measures this)
- Gum recession around the implant, the implant looks “longer”
- Radiographic bone loss around the implant compared with baseline (seen on X-rays)
- In later stages, the crown or implant may feel loose
A really important point: pain is not required. Many people describe it in vague, real-life language like “pressure but not loose,” “it feels weird when I bite,” or “it just feels off.” That is why routine maintenance and measurements matter.
What each sign or symptom usually means (quick explanations)
People often describe these in very normal, real-world language like “my floss comes out with blood,” “the gum looks angry,” “it tastes gross near that implant,” or “it feels like pressure but not loose.” Here is how we interpret those symptoms.
Bleeding around the implant when brushing or flossing
If bleeding keeps happening after the healing phase, it is a sign of inflammation. It does not automatically prove peri-implantitis, but it is a common early red flag that deserves an exam.
Swollen, puffy, or red gum tissue around the implant
Healthy implant gums should look calm and feel firm. Ongoing redness or puffiness usually means inflammation, often because plaque is being trapped somewhere or cleaning access is tougher than it looks.
Pus, discharge, or a persistent bad taste
Pus is a stronger warning sign than bleeding alone. Patients often describe “a gross taste” or noticing discharge when they press the gumline. This is one of the signs that should move you up the priority list for an appointment.
Deepening pockets around the implant (your dentist measures this)
This is not something you can measure at home, but it is one of the big clinical clues. If pockets are getting deeper compared with previous visits, we start worrying more about peri-implantitis, especially if there is bleeding or pus.
Gum recession around the implant, the implant looks longer
People often say, “I can see more metal now.” Recession can have different causes, but when it shows up with bleeding or swelling, we want to evaluate the tissues and bone support.
The implant crown feels “high,” “different,” or uncomfortable to bite on
This is a common complaint: “It feels weird when I bite.” Bite overload and mechanical issues can contribute to irritation and make inflammation harder to control, so we check the bite, the crown, and the implant tissues.
The crown or implant feels loose
This is urgent. Sometimes it is only a loose screw or crown, but sometimes it signals advanced loss of support. Either way, it should be assessed promptly.
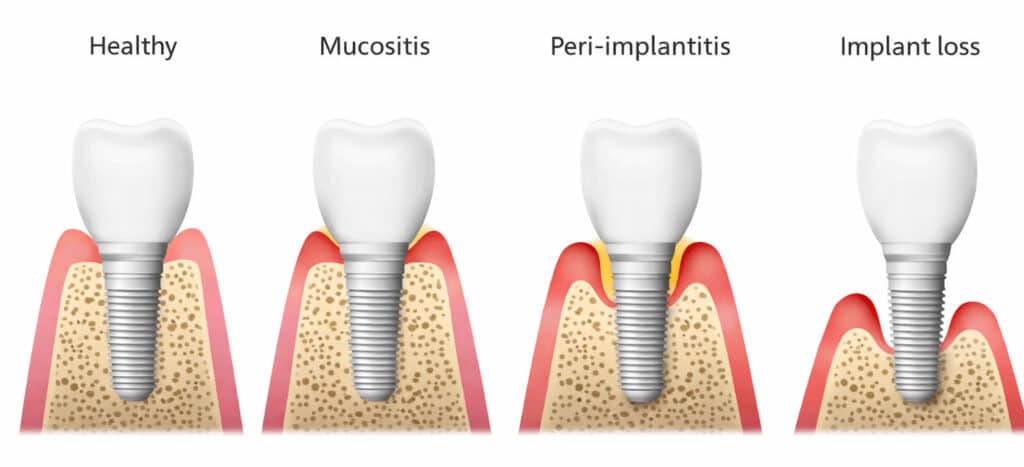
Peri-implant mucositis vs peri-implantitis
People often ask this in one sentence: “Is this just irritated gums or am I going to lose my implant?”
Peri-implant mucositis
Inflammation around the implant is similar to gingivitis around teeth. You can see bleeding on gentle probing and swelling, but there is no progressive bone loss after initial healing. This stage is often reversible when caught early.
Peri-implantitis
Inflammation around the implant plus progressive loss of supporting bone. Clinically, we see bleeding and or pus on probing, deepening pockets and or recession, and bone loss on X-rays.
Risk factors and prevention
Patients often tell me, “I brush, I floss, I don’t get it.” And honestly, a lot of peri-implantitis cases are not caused by one single thing. It is usually plaque plus one or more risk factors that make inflammation easier to trigger or harder to control.
Common risk factors
- History of gum disease (periodontitis), which increases susceptibility around implants
- Inconsistent plaque control around the implant due to access or crown contours
- Smoking
- Diabetes and other health factors that can affect inflammation and healing
- Maintenance gaps (skipping professional implant checks and cleanings)
Practical prevention tips (what actually helps)
- Clean like you mean it, but gently: brush the gumline and use the interproximal tools that suit your implant restoration
- Ask for an implant-specific hygiene plan: floss, super floss, interdental brushes, water flosser, it depends on the crown design
- Keep regular maintenance visits: probing and occasional X-rays help spot changes early
- If you smoke, reducing helps: smoking is a known risk factor for peri-implant disease
- If you have diabetes, aim for good control: overall inflammation control matters
What happens at the appointment
This section matters for conversions and for patient comfort, because a lot of people come in worried they’ll be judged, or that they’re “overreacting” because the symptoms feel small. You’re not. With implants, tiny changes like bleeding, puffiness, or a weird taste are exactly the kind of early signals we want to catch before they turn into something bigger.
A typical peri-implant assessment usually looks like this:
A quick chat about symptoms and timing
We’ll ask what you’re noticing and when it started. Patients often describe things like “my floss comes out with a bit of blood,” “it tastes gross near that tooth,” “it feels like pressure but not loose,” or “it just started feeling off when I bite.” We’ll also ask about recent triggers, like a missed cleaning, a new medication, illness, stress, clenching, or changes in home care tools.
A careful look at the gums and how the crown sits
We check the gum tissue for redness, puffiness, recession, and any spots that look irritated or difficult to keep clean. We also look at the shape of the implant crown, because sometimes the issue is not effort, it’s access. If the restoration has contours that trap plaque, you can be doing your best and still struggle.
Gentle probing around the implant
This is one of the most important parts. We lightly measure around the implant to check for bleeding, pus, and pocket depths. It’s quick and usually well tolerated. The goal is not to “poke around for fun,” it’s to get a baseline and see whether anything has changed compared to past readings.
X-rays to check bone levels
X-rays help us see whether there is bone loss around the implant and whether it’s stable or progressing. If you’ve had previous X-rays, comparing over time is huge, because peri-implantitis is defined by inflammation plus progressive bone loss, not just a sore spot one day.
A crown and bite check
We’ll check whether the crown is stable and whether the bite is hitting that implant too heavily. If the bite is high or you clench or grind, it can add stress and make it harder to calm the tissues. We also check for any looseness in components because a loose crown or screw can create gaps that trap bacteria and irritate the gums.
A clear plan and what you can do right away
Before you leave, you should know what stage you’re in (healthy, mucositis, or peri-implantitis), what the next step is, and what to do at home. That might be targeted cleaning instructions, a specific tool recommendation, professional cleaning around the implant, or referral for more advanced treatment if needed.
What patients love hearing: diagnosis is not based on vibes. It’s based on measurements over time, how the tissues respond, and what your X-rays show.
Myths and misconceptions about peri-implantitis
Myth 1: If it does not hurt, it is fine
Not true. Early peri-implant disease can be quiet. Bleeding and swelling can show up before pain.
Myth 2: Bleeding once means implant failure
Usually not. One-off bleeding can happen with food impaction or aggressive cleaning. Persistent bleeding is the issue.
Myth 3: Antibiotics fix peri-implantitis on their own
Antibiotics may be used in some cases, but they do not replace removing plaque and deposits and addressing crown design or pocket issues.
Myth 4: Implants do not get gum disease
They can. The tissue around implants can inflame similarly to gum disease around teeth, and peri implantitis includes bone loss.
Myth 5: It is always your fault
Not true. Home care matters a lot, but restoration design, access, past periodontal history, and health factors also play real roles.
When to book urgently
If you have any of the following, do not wait for your next cleaning:
- Pus or discharge
- Rapid swelling or increasing pain
- Persistent foul taste or odour that keeps returning
- A loose crown or any feeling of movement
- Bleeding that is frequent and getting worse
What treatment can look like
Patients often worry that treatment automatically means surgery. Not always. The plan depends on how deep the pockets are, whether bone loss is present, and whether the crown design is contributing.
Treatment may include professional debridement, improved home care coaching, addressing plaque traps, bite adjustment when appropriate, and, in more advanced cases, surgical therapy to access and manage the infected area and bone defect.
What you can safely do at home while you wait
A very common online question is: “Am I making it worse by cleaning it?” In most cases, the answer is no, you are helping, as long as you are gentle.
- Brush gently but thoroughly twice daily, aiming at the gumline
- Clean between teeth and around the implant using the method your dental team recommended
- Warm salt water rinses can help comfort
- Avoid smoking
- Avoid poking or digging at the gumline
If you are seeing pus, significant swelling, or looseness, focus on getting seen promptly rather than trying home fixes.
Frequently Asked Questions (FAQ)
Check us out on Facebook and Twitter for daily information about Oral Health from Martindale Dental, or visit our offices in Hamilton and St. Catharines.
Have more questions?
Please contact us for all inquiries or to book an appointment with one of our convenient clinic locations. We look forward to hearing from you.