Do you feel heartburn often or notice your teeth hurting when you eat? These could be signs of acid reflux, or GERD, a condition that damages more than your stomach—it harms your teeth and gums, too. Acid reflux can erode enamel, cause sensitivity, and lead to cavities, gum disease, and bad breath, affecting your smile and confidence. In this article, we explore five key ways acid reflux impacts your oral health and how a dentist for acid reflux tooth damage can help. At Martindale Dental in Hamilton and St. Catharines, we’re here to protect your teeth from GERD’s effects with expert care.
Table of Contents
What Is Acid Reflux and How Does It Affect Your Oral Health?
Acid reflux happens when stomach acid flows back into the esophagus, often reaching the mouth, where it can damage teeth and gums. Known as GERD when chronic, this condition affects about 20% of adults, per the Canadian Dental Association. The acid’s low pH (around 2.0) erodes tooth enamel, the hard outer layer protecting your teeth (Healthline). This can lead to sensitivity, cavities, and gum issues, while symptoms such as a sour taste or bad breath may signal oral health risks. For example, you may experience pain with hot drinks or notice yellowing of your teeth. An oral health checkup for GERD patients can help identify these problems early, allowing you to maintain a healthy smile.
Why Does Acid Reflux Harm Teeth?
Acid reflux, also known as gastroesophageal reflux disease (GERD), can harm teeth and gums by eroding enamel, reducing saliva production, and irritating the gums, leading to cavities, sensitivity, and gum disease. Stomach acid (pH ~2.0) from reflux episodes softens enamel, exposing sensitive dentin and increasing decay risk. Nighttime reflux worsens damage due to lower saliva production. GERD medications, such as proton pump inhibitors, can cause dry mouth, which limits the saliva’s ability to neutralize acid and clear debris, leading to plaque buildup and bad breath. Acid also irritates the gums, causing redness or bleeding, which can signal gum disease and increase the risk of tooth loss. These effects underscore the importance of dental care in managing acid reflux, tooth erosion, and related issues. Key reasons include:
- Enamel Erosion: Acid softens enamel, making teeth thinner and more prone to cavities.
- Dry Mouth: Medications reduce saliva, fostering bacteria and decay.
- Gum Inflammation: Acid causes red, bleeding gums, increasing gum disease risk.
- Bacterial Growth: Acid and dry mouth promote bacteria, worsening oral health.
How Acid Reflux Damages Your Teeth: 5 Key Impacts
Acid reflux and GERD pose a threat to oral health by eroding enamel, damaging gums, and compromising overall tooth structure. Below are five key ways acid reflux affects your teeth and gums, with details on symptoms and dental solutions.
1. Tooth Erosion from Acid Reflux
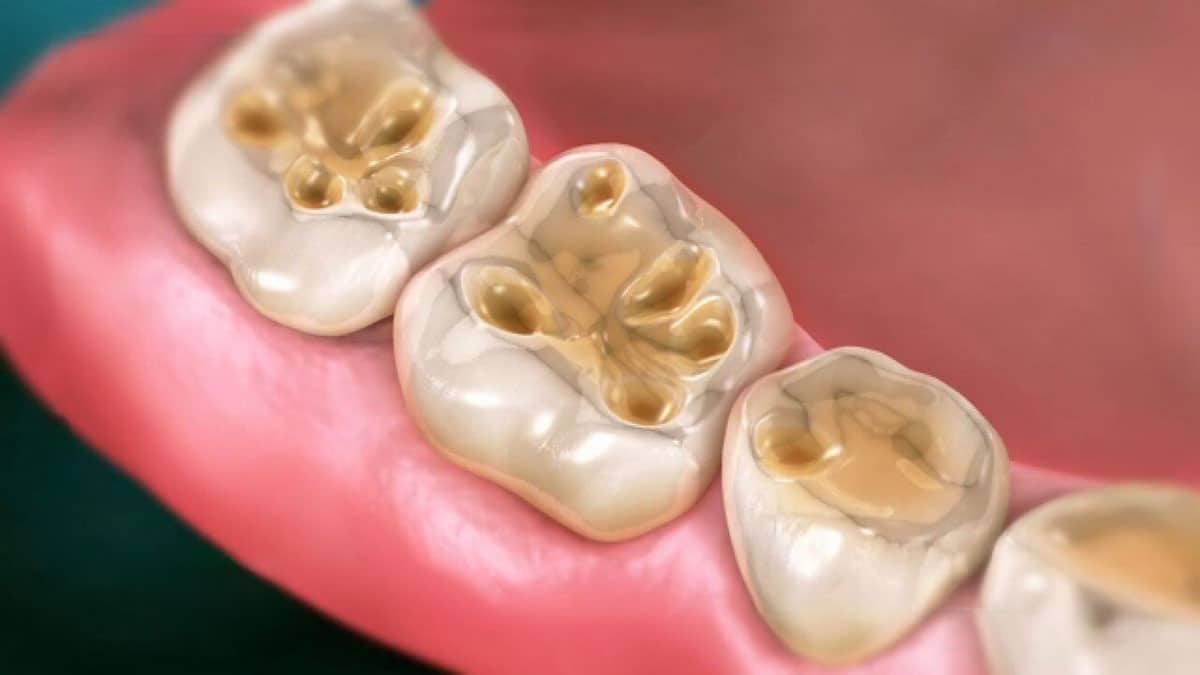
Tooth erosion is a primary way acid reflux damages teeth, as stomach acid gradually wears away at the enamel, leaving the teeth vulnerable to further harm. This process, driven by GERD’s acidic surges, affects up to 40% of patients, making it a widespread concern. Eroded enamel can lead to sensitivity, cavities, and cosmetic issues, impacting your smile and confidence (PMC). Recognizing the signs and seeking dental care early can prevent long-term damage. Below, we explore what causes tooth erosion, its key symptoms, and how dentists treat GERD and tooth enamel damage to restore and protect your teeth.
What Causes Tooth Erosion?
Acid reflux exposes teeth to stomach acid, which erodes enamel over time, weakening the tooth’s structure. Here’s how GERD contributes:
Acidic Exposure: During reflux episodes, stomach acid with a low pH (around 2.0) contacts teeth, softening and dissolving enamel. For example, frequent heartburn after meals can repeatedly bathe teeth in acid.
Nighttime Reflux: Acid reflux at night, common in GERD patients, prolongs acid exposure, as saliva production decreases during sleep, reducing natural protection.
Dietary Factors: Consuming acidic foods or drinks, such as citrus or soda, by GERD patients can exacerbate enamel erosion, thereby compounding the effects of stomach acid.
Symptoms of Tooth Erosion
Tooth erosion from acid reflux shows distinct signs, indicating the need for dental intervention. Look for these symptoms:
Yellowing Teeth: Thinning enamel reveals the yellow dentin layer underneath, making teeth appear discoloured or aged.
Rounded Edges: Teeth lose their sharp, defined edges, appearing worn or smooth, often noticeable on front teeth.
Translucency: Front teeth may look see-through at the edges, a sign of significant enamel loss, affecting your smile’s appearance.
Increased Sensitivity: Eroded enamel causes discomfort with hot, cold, or sweet foods, as dentin becomes exposed to stimuli.
How Dentists Treat Erosion
Dentists offer targeted treatments to repair and prevent further tooth erosion, helping GERD patients maintain healthy teeth. These solutions include:
Fluoride Treatments: Professional fluoride varnish or gel applications strengthen remaining enamel, making it more resistant to acid. Applied during checkups, fluoride helps remineralize teeth.
Dental Bonding: Tooth-colored resin is applied to eroded surfaces to restore shape and appearance. Bonding is ideal for repairing chipped or translucent teeth.
Restorative Options: For severe erosion, crowns or veneers protect and rebuild damaged teeth, ensuring durability and aesthetics.
Regular Checkups: Routine dental visits every six months allow dentists to monitor erosion and apply preventive measures, like sealants, to shield teeth.
If you notice signs of acid reflux in teeth, like shiny or rounded surfaces, a dentist can help. In Toronto, our team at [Your Dental Practice Name] offers solutions to treat tooth erosion from GERD.
2. Tooth Sensitivity Due to GERD

Can acid reflux make your teeth hurt? Yes, tooth sensitivity from acid reflux occurs when stomach acid erodes the enamel, exposing the dentin and causing pain during everyday activities such as eating or drinking. This discomfort, often sharp or sudden, can make enjoying meals challenging and signal that GERD is causing damage to your teeth. For GERD patients, sensitivity is a common issue that affects quality of life, but dentists can offer practical solutions to manage it. Below, we explore why sensitivity occurs, key signs to recognize, and dental strategies to alleviate tooth sensitivity caused by acid reflux, helping you protect your smile.
Why Does Sensitivity Happen?
Acid reflux triggers tooth sensitivity by eroding enamel, leaving dentin vulnerable to external stimuli. Here’s how GERD contributes:
Enamel Erosion: Stomach acid from reflux episodes softens and wears away enamel, the tooth’s protective outer layer. This exposes dentin, a softer layer with nerve-connected tubules, causing sensitivity.
Frequent Acid Exposure: Regular heartburn or regurgitation, especially at night, bathes teeth in acid, accelerating enamel loss. For example, GERD patients might notice sensitivity after acidic meals.
Dry Mouth Effects: GERD medications, like proton pump inhibitors, often reduce saliva, which normally buffers acid and protects enamel. Dry mouth worsens sensitivity by leaving teeth exposed.
Signs of Sensitivity
Tooth sensitivity due to GERD manifests in distinct ways, indicating the need for dental care. Look for these symptoms:
Pain with Temperature: Discomfort or sharp pain when consuming hot or cold foods, like soup or iced tea, suggests exposed dentin from acid reflux.
Sweet Sensitivity: Pain or stinging when eating sugary snacks, such as candy or pastries, indicates enamel loss, a common GERD effect.
Brushing Discomfort: Sensitivity or wincing during brushing, especially with cold water, shows dentin sensitivity, making oral hygiene challenging.
General Tooth Ache: A lingering ache or discomfort in multiple teeth, particularly after acidic foods, signals ongoing GERD-related damage.
Dental Solutions for Sensitivity
Dentists provide targeted treatments and advice to manage GERD-related tooth sensitivity, restoring comfort and protecting teeth. These solutions include:
Desensitizing Toothpaste: Products like Sensodyne block nerve signals, reducing pain from hot, cold, or sweet stimuli. Use twice daily for best results(The 247 Dentist).
Fluoride Varnish: Professional fluoride applications remineralize enamel, strengthening it against acid and shielding dentin. Dentists apply varnish during checkups.
Avoiding Triggers: Limit acidic foods and drinks, like citrus, soda, or tomatoes, to reduce reflux and enamel erosion. Opt for smaller, less spicy meals.
Protective Sealants: Dental sealants coat teeth, creating a barrier against acid, ideal for preventing further sensitivity in GERD patients.
3. Increased Risk of Cavities from GERD
Acid reflux significantly increases the risk of cavities by weakening tooth enamel and reducing saliva, thereby creating an environment that fosters decay. GERD’s acidic surges soften enamel, making it easier for bacteria to cause cavities, while dry mouth from medications exacerbates the problem. These factors contribute to plaque buildup and tooth damage caused by acid reflux, potentially compromising your smile. Regular dental care is essential for preventing and treating cavities caused by GERD. Below, we explore how GERD leads to cavities, key symptoms to watch for, and effective prevention and treatment strategies to protect your oral health.
How GERD Leads to Cavities
GERD increases cavity risk through acid exposure and reduced saliva, both of which harm teeth. Here’s how it happens:
Acid-Softened Enamel: Stomach acid from reflux episodes softens enamel, the tooth’s protective layer, making it easier for bacteria to penetrate and cause decay. For example, frequent heartburn after meals can weaken teeth over time.
Dry Mouth from Medications: Certain medications used to treat GERD, such as proton pump inhibitors, can reduce saliva production, leading to dry mouth. Saliva normally neutralizes acids and clears food debris, so its absence allows plaque to build up.
Plaque Buildup: The combination of weakened enamel and low saliva creates a breeding ground for bacteria, leading to sticky plaque that erodes teeth and forms cavities.
Symptoms of Cavities
Cavities caused by GERD show distinct signs, indicating the need for dental attention. Look for these symptoms:
Dark Spots: Small pits, stains, or dark spots on teeth signal early decay, often visible on molars or front teeth.
Tooth Pain: Aching or sharp pain when chewing or biting suggests a cavity has reached deeper tooth layers.
Sensitivity: Increased discomfort with sweets, cold drinks, or hot foods indicates enamel loss, common in GERD patients.
Rough Texture: Teeth may feel rough or uneven as cavities form, noticeable when running your tongue over surfaces.
Preventing and Treating Cavities
Dentists offer solutions to prevent and treat cavities, helping GERD patients maintain healthy teeth. These strategies include:
Sealants: Dental sealants coat teeth, creating a barrier against acid and bacteria, ideal for protecting molars from GERD-related decay.
Fillings: Composite resin fillings repair early cavities, restoring tooth structure and preventing further damage. Dentists remove decayed areas and fill them for durability.
Saliva Stimulation: Chewing sugar-free gum, especially xylitol-based, boosts saliva to neutralize acid and clear debris, reducing cavity risk.
Fluoride Treatments: Professional fluoride applications strengthen enamel, helping it resist GERD’s acidic effects and prevent cavities.
4. Gum Disease Linked to Acid Reflux

Acid reflux and gum disease are linked, as acid exposure and dry mouth increase the risk of periodontitis, a serious gum infection.
Why GERD Affects Gums
Acid irritates gums, causing inflammation, while dry mouth from GERD medications allows bacteria to thrive. This leads to gum disease, with symptoms like bleeding or swollen gums. Untreated, it can cause tooth loss.
Signs of Gum Disease
Acid reflux exacerbates gum disease, or periodontitis, by promoting bacterial growth through acid exposure and dry mouth caused by GERD medications. If you have GERD, you may notice changes in your gums that signal this condition, especially if you experience frequent heartburn or a sour taste in your mouth. Early recognition can prevent serious issues like tooth loss, prompting a visit to a dentist for acid reflux and tooth damage. Here are the key signs to watch for:
- Bleeding Gums: Blood when brushing or flossing indicates inflammation caused by acid irritation and bacterial infection. For example, seeing pink streaks after brushing may suggest gum disease, which a dentist can treat early to prevent progression.
- Swollen Gums: Red, puffy gums feel tender due to acid and bacterial buildup. You might notice discomfort when chewing or sensitivity, signalling the need for dental care to reduce inflammation.
- Receding Gums: Gums pulling back make teeth appear longer, as acid weakens tissue and bacteria erode the gumline. This exposes roots, causing sensitivity, and requires prompt treatment to prevent tooth loss.
- Persistent Bad Breath: Chronic bad breath, often accompanied by a sour taste associated with gastroesophageal reflux disease (GERD), can be a sign of gum disease. Bacteria in inflamed gums cause halitosis, treatable with professional dental care.
Dental Treatments for Gum Disease
Dentists treat gum disease worsened by acid reflux with procedures to remove bacteria, reduce inflammation, and restore gum health. These treatments are vital for GERD patients to prevent tooth loss and maintain oral health. Here are the main options to address acid reflux and gum disease:
- Professional Cleanings: Dental cleanings remove plaque and tartar that worsen gum inflammation in GERD patients. A hygienist uses tools to clear deposits, reducing swelling and bleeding. Cleanings every six months help control bacteria.
- Scaling and Root Planing: This deep cleaning treats advanced gum disease by removing tartar below the gumline and smoothing roots to prevent bacterial reattachment. It helps gums heal and reduces pockets, ideal for GERD-related gum issues.
- Antimicrobial Rinses: Prescribed rinses like chlorhexidine target bacteria, reducing infection and supporting gum recovery. These are gentle, avoiding worsening dry mouth from GERD medications.
- Preventive Guidance: Dentists advise rinsing with water after reflux, using fluoride toothpaste, and chewing sugar-free gum to boost saliva. Avoiding acidic foods also helps protect gums.
5. Bad Breath and Other Oral Symptoms

Bad breath from acid reflux, along with a sour taste in the mouth, is a common oral symptom signalling GERD’s impact on dental health. These issues, often embarrassing, can affect your confidence and social interactions, while other symptoms, such as tooth discoloration or a burning sensation, highlight the broader effects of acid reflux on oral health.
If you’re experiencing these signs, GERD may be harming your teeth and gums, and a dentist can help. Below, we explore the causes, related symptoms, and methods for managing these oral health challenges to protect your smile.
Causes of Bad Breath and Sour Taste
Acid reflux creates an acidic oral environment that fosters bacterial growth, leading to persistent bad breath, or halitosis, and a sour taste in the mouth. Here’s how GERD contributes:
- Bacterial Growth: Stomach acid from reflux episodes coats the mouth, promoting bacteria that release foul-smelling compounds. For example, you may notice bad breath even after brushing, especially after meals, which can trigger reflux.
- Regurgitation: Acid flowing back into the mouth leaves a sour or metallic taste, which is often exacerbated by lying down or consuming spicy foods. This taste can linger, affecting your enjoyment of food.
- Dry Mouth: GERD medications, such as proton pump inhibitors, reduce saliva, which can worsen bad breath and a sour taste by allowing bacteria to thrive. Dry mouth also increases cavity risk.
Other Oral Symptoms
Beyond bad breath and sour taste, acid reflux causes additional oral symptoms that signal GERD’s dental impact:
- Burning Sensation: Acid irritates the mouth, tongue, or throat, causing a burning sensation, especially after episodes of reflux. You might feel discomfort when swallowing or speaking.
- Dry Mouth: Reduced saliva from GERD medications or acid exposure leaves the mouth sticky or parched, increasing decay and gum disease risk.
- Tooth Discoloration: Enamel erosion from acid causes yellowing or translucency, making teeth look worn. This can make you self-conscious about your smile.
- Tooth Sensitivity: Eroded enamel exposes dentin, causing pain with hot, cold, or sweet foods, often paired with bad breath or sour taste.
Managing Oral Symptoms
Dentists can help manage these GERD-related oral symptoms with targeted strategies to reduce bacteria, neutralize acid, and protect your oral health. Here are effective approaches:
- Tongue Brushing: Brush your tongue daily with a soft toothbrush to remove bacteria causing bad breath. This simple step can significantly improve oral freshness.
- Alcohol-Free Mouthwash: Use a gentle, alcohol-free mouthwash to neutralize acid and reduce bacteria without worsening dry mouth. Look for products with fluoride for added protection.
- Hydration: Drink water frequently to dilute acid, combat dry mouth, and promote saliva flow. Keep a water bottle handy, especially after reflux episodes.
- Saliva-Stimulating Products: Chew sugar-free gum or use lozenges to boost saliva, which helps wash away acid and bacteria, reducing bad breath and sour taste.
- Regular Dental Checkups: Visit a dentist every six months to monitor GERD’s oral effects, like enamel erosion or gum issues, and receive treatments like fluoride applications.
If you’re asking, “Why are my teeth eroding?” or noticing a sour taste in the mouth, GERD could be the culprit. A dentist can evaluate and address these symptoms.
How Dentists Can Help with GERD-Related Tooth Issues

Dentists play a vital role in managing GERD’s impact on oral health, offering treatments and guidance to protect your teeth and gums from acid reflux damage. During routine exams, they identify signs of acid reflux in teeth, such as worn enamel, tooth sensitivity, or gum inflammation, and provide solutions to restore your smile. By addressing these issues early, dentists help prevent long-term damage like cavities or tooth loss, making an oral health checkup for GERD patients essential. Below, we explore how dentists diagnose, treat, and prevent GERD-related tooth issues, ensuring comprehensive care for those with acid reflux.
Diagnostic Role
Dentists are often the first to spot GERD’s oral effects, guiding patients toward proper care. Their expertise helps catch issues early, preventing further damage.
- Spotting Signs: Dentists notice eroded enamel, tooth sensitivity, or swollen gums during exams. For example, they may see shiny, yellowed teeth or inflamed gums, signalling acid reflux’s impact.
- Referrals: If GERD is suspected, dentists refer patients to a gastroenterologist for systemic management, ensuring holistic treatment. They may ask about heartburn or a sour taste to confirm suspicions.
- Symptom Assessment: Dentists evaluate symptoms like bad breath or a burning sensation in the mouth, linking them to GERD and recommending dental solutions.
Treatment Options
Dentists offer targeted treatments to repair GERD-related damage and strengthen oral health, tailored to each patient’s needs.
- Fluoride Applications: Professional fluoride varnish or gel strengthens enamel, helping it resist acid erosion (PMC). This is ideal for patients with early enamel wear from GERD.
- Restorations: Dental bonding or crowns repair eroded or chipped teeth. For instance, bonding restores a tooth’s appearance, while crowns protect severely damaged teeth.
- Gum Care: Cleanings or scaling and root planing treat gum disease caused by GERD, removing plaque and reducing inflammation to prevent tooth loss.
Preventive Strategies
Dentists provide practical advice to minimize GERD’s oral health effects, empowering patients to protect their teeth.
- Rinsing Advice: Rinse with water or a baking soda solution after reflux to neutralize acid and protect enamel. This simple step reduces erosion risk.
- Oral Hygiene: Use fluoride toothpaste and floss daily to strengthen teeth and prevent cavities. Chewing sugar-free gum boosts saliva, counteracting dry mouth.
- Diet Tips: Avoid acidic foods like citrus or soda and eat smaller meals to reduce reflux frequency, helping maintain oral health.
Tips to Protect Your Teeth from Acid Reflux

Protecting your teeth from acid reflux requires daily habits and professional dental care to shield your smile from GERD’s damaging effects. Acid reflux, with its acidic surges, can erode enamel, cause sensitivity, and increase gum disease risk, but simple strategies can minimize these impacts. By adopting these practices, you can reduce tooth damage and maintain oral health, even with frequent heartburn or a sour taste in the mouth. Below, we share seven practical tips to help you safeguard your teeth, emphasizing how to protect teeth from acid reflux and the importance of regular dental visits.
Daily Habits to Prevent Tooth Damage
These everyday practices help neutralize acid, strengthen teeth, and reduce GERD’s oral health effects, keeping your smile healthy.
- Rinse After Reflux: Rinse your mouth with water or a baking soda solution (1 teaspoon in a glass of water) after a reflux episode to neutralize stomach acid. This prevents enamel erosion and reduces sensitivity. For example, if heartburn strikes after dinner, a quick rinse can protect your teeth before brushing.
- Choose Fluoride Toothpaste: Brush twice daily with fluoride toothpaste, like Sensodyne Pronamel, the best toothpaste for GERD patients. Fluoride strengthens enamel, making it more resistant to acid. Look for products designed to repair early enamel damage, ideal for those with GERD.
- Chew Sugar-Free Gum: Chew sugar-free gum for 20 minutes after meals to stimulate saliva, which washes away acid and bacteria. Saliva also neutralizes acid, reducing dry mouth and cavity risk. Choose xylitol-based gum for added antibacterial benefits.
- Delay Brushing: Wait 30 minutes after a reflux episode to brush, as acid softens enamel, making it vulnerable to abrasion. Brushing too soon can worsen erosion, so rinse first and brush later to protect your teeth.
Lifestyle and Professional Care
These strategies combine lifestyle changes and dental visits to manage GERD and protect your oral health long-term (NIDDK).
- Stay Hydrated: Drink water throughout the day to dilute acid in the mouth and combat dry mouth, a common GERD medication side effect. Keeping a water bottle handy, especially at night, helps maintain saliva flow and reduces bacterial growth.
- Manage GERD Symptoms: Work with your doctor to control acid reflux through diet (e.g., avoiding spicy or acidic foods like tomatoes), medications (e.g., proton pump inhibitors), or lifestyle changes like sleeping with your head elevated. Reducing reflux frequency protects your teeth and gums.
- Schedule Dental Checkups: Visit your dentist every six months for an oral health checkup for GERD patients. Dentists can spot signs of acid reflux in teeth, like enamel wear or gum inflammation, and offer treatments such as fluoride applications or cleanings to prevent damage.
When to See a Dentist for Acid Reflux
Knowing when to see a dentist for acid reflux is crucial to prevent long-term damage to your teeth and gums caused by GERD’s acidic effects. Acid reflux can erode enamel, cause sensitivity, and trigger gum disease, but early dental care can stop these issues from worsening. Symptoms like a sour taste, bad breath, or frequent heartburn may signal that GERD is affecting your oral health, requiring professional attention. Below, we outline key signs that indicate it’s time for an oral health checkup for GERD patients, helping you protect your smile with timely intervention.
Oral Health Symptoms to Watch For
These symptoms suggest GERD is damaging your teeth or gums, signaling the need for a dentist’s evaluation.
Tooth Sensitivity: Pain or discomfort when eating hot, cold, or sweet foods indicates enamel erosion from acid reflux. For example, you might wince when drinking iced coffee or eating candy, a sign that GERD is weakening your teeth’s protective layer.
Sour Taste or Bad Breath: Persistent sour taste in the mouth or bad breath from acid reflux can point to GERD’s oral impact. A lingering metallic taste after meals or chronic halitosis, even after brushing, warrants a dental checkup.
Bleeding Gums: Gums that bleed when brushing or flossing suggest gum disease linked to acid reflux. Acid irritation and bacterial growth from dry mouth can inflame gums, causing redness or tenderness.
Worn Teeth: Yellowing, translucent, or rounded teeth show enamel wear from GERD. You might notice teeth looking thinner or more see-through at the edges, a sign of acid damage needing dental repair.
GERD-Related Indicators
Systemic GERD symptoms also signal the need for dental care to protect your oral health.
Frequent Heartburn: Experiencing heartburn more than twice a week indicates chronic GERD, which increases oral health risks. Regular acid reflux episodes can erode teeth and gums, requiring a dentist’s monitoring.
Difficulty Swallowing: Trouble swallowing or a feeling of food stuck in the throat, often tied to GERD, can accompany oral symptoms like sensitivity or bad breath, prompting a dental visit.
Chronic Dry Mouth: Dry mouth resulting from GERD medications or acid exposure reduces saliva production, increasing the risk of cavities and gum disease. If your mouth feels sticky or parched, a dentist can help.
A dentist for acid reflux tooth damage can assess these symptoms and offer treatments like fluoride or cleanings. At Martindale Dental in Hamilton and St. Catharines, our team provides expert care for GERD-related oral issues. Schedule an appointment to safeguard your teeth and gums.
Quick Takeaways
Acid reflux can lead to significant dental erosion if left unmanaged.
Early detection by a dentist can prevent severe oral health issues.
Combining medical treatment for GERD with proper oral hygiene is essential.
Lifestyle changes play a pivotal role in managing both GERD and oral health
Final Thoughts on Protecting Your Smile from Acid Reflux
Acid reflux, or GERD, is more than just a digestive concern—it poses a significant threat to your oral health. The backflow of stomach acids can erode tooth enamel, leading to sensitivity, discoloration, and increased vulnerability to cavities. Recognizing the signs early and implementing preventive measures are crucial steps in safeguarding your smile.
Maintaining a proactive approach involves:
- Regular Dental Check-ups: Dentists can detect early signs of enamel erosion and provide guidance on protective strategies.
- Effective Oral Hygiene Practices: Using fluoride toothpaste, waiting at least 30 minutes after acid exposure before brushing, and rinsing with water can help minimize damage.
- Dietary Adjustments: Limiting acidic foods and beverages and avoiding eating close to bedtime can reduce acid reflux episodes.MouthHealthy
- Lifestyle Modifications: Elevating the head during sleep, maintaining a healthy weight, and refraining from smoking are beneficial in managing GERD symptoms.
By integrating these practices into your daily routine, you not only address the discomfort associated with acid reflux but also fortify your oral health against its detrimental effects. Remember, a collaborative approach involving both your dentist and healthcare provider ensures comprehensive care. Take charge of your health today to preserve your radiant smile for years to come.
A dentist can assess erosion patterns and may inquire about GERD symptoms to determine the cause.
Enamel loss is permanent, but treatments can restore function and appearance.
Yes, children with GERD can experience enamel erosion; pediatric dental check-ups are important.
References
American Dental Association. “Tooth Erosion and Acid Reflux.”
https://www.mouthhealthy.org/all-topics-a-z/tooth-erosionHealthline. “GERD Teeth: Signs of Dental Erosion and Prevention.”
https://www.healthline.com/health/gerd-teethNational Institute of Diabetes and Digestive and Kidney Diseases. “Acid Reflux (GER & GERD) in Adults.”
https://www.niddk.nih.gov/health-information/digestive-diseases/acid-reflux-ger-gerd-adultsThe 247 Dentist. “Signs of Acid Reflux on Teeth: Prevention & Solutions.”
https://the247dentist.com/signs-of-acid-reflux-on-teeth/West Bowmanville Family Dental. “GERD and Its Effect on Oral Health.”
https://www.westbowmanvilledental.com/gerd-and-its-effect-on-oral-health/PMC. “Dental Approach to Erosive Tooth Wear in Gastroesophageal Reflux Disease.”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4245552/Colgate. “10 Ways to Keep Acid Reflux From Damaging Teeth.”
https://www.colgate.com/en-us/oral-health/gastrointestinal-disorders/10-ways-to-keep-acid-reflux-from-damaging-teethDental Health. “Mystery Solved: Acid Reflux and the Oral Cavity.”
https://www.oralhealthgroup.com/features/mystery-solved-acid-reflux-and-the-oral-cavity/Winnipeg Dental Group. “How Acid Reflux Affects Oral Health.”
https://winnipegdentalgroup.ca/how-acid-reflux-affects-oral-health/
Check us out on Facebook and Twitter for daily information about Oral Health from Martindale Dental, or visit our offices in Hamilton and St. Catharines.
Have more questions?
Please contact us for all inquiries or to book an appointment with one of our convenient clinic locations. We look forward to hearing from you.

