Oral Surgery in Hamilton
Treating dental issues including impacted teeth, jaw disorders, and facial injuries.
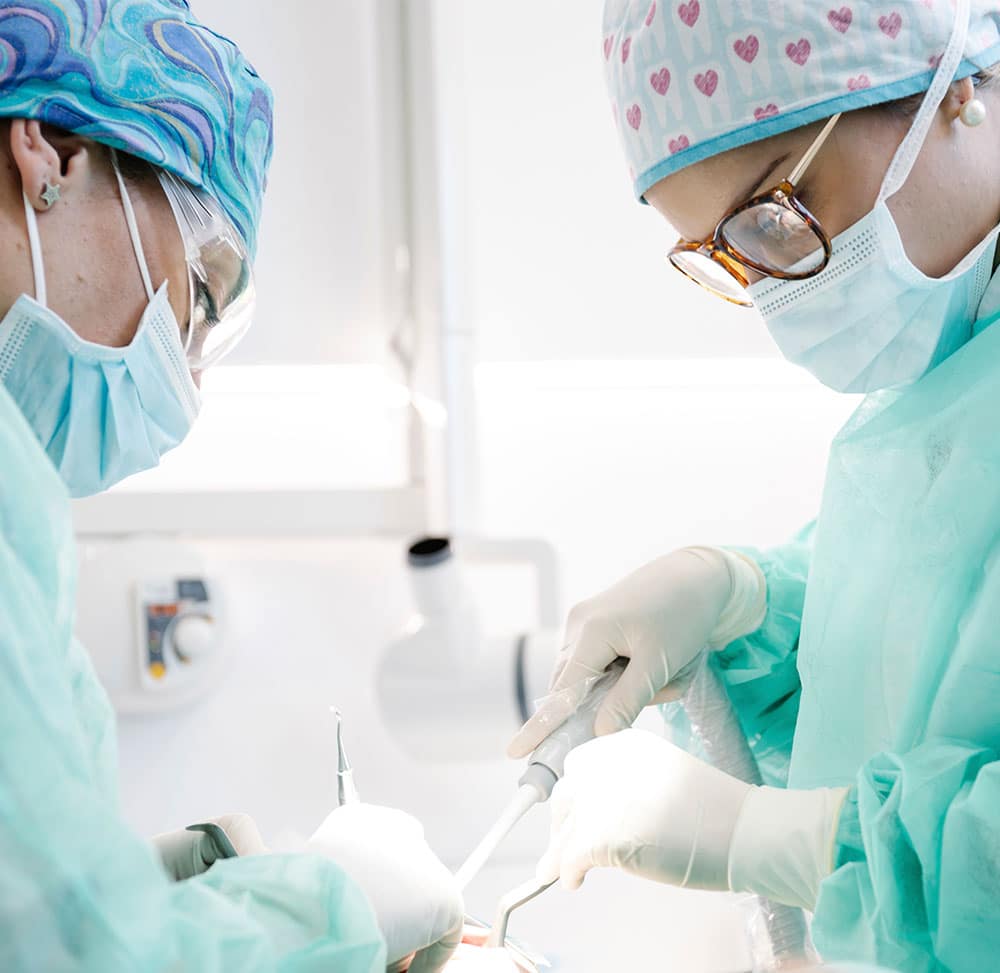

Resolve problems.
Improve your smile.
Oral Surgery
in Hamilton
Treating dental issues including impacted teeth, jaw disorders, and facial injuries.

What is oral surgery in Hamilton?
Oral surgery is an advanced branch of modern dentistry whose purpose is to treat patients who require procedures outside of the normal scope of a dental practice. This includes everything from tooth extractions to jaw reconstruction surgery. TMJ disorders, cleft lip and palate, diseases and tumors or sleep apnea are also common reasons patients are referred to an oral surgeon in Hamilton.
Oral surgery describes any surgery that takes place on the tissue of your mouth (teeth and gums). Maxillofacial surgery is a closely related term you might hear as it encompasses the entire jaw, face and head.
At Martindale Dental, your Jackson Square dental team, we rely on our 20+ years of experience treating all kinds of oral surgery cases in Hamilton.

Why oral surgery might be necessary
Typical treatments at your dentist include (but are not limited to) teeth cleanings, fillings, crowns, sealants, root canals bridges, gum care, dental exams and x-rays. If more serious procedures are required, such as wisdom teeth removal, soft tissue removal, dental implants, facial trauma care, tumour removal, TMJ treatments and more – an oral surgeon may be required to help. Your dentist will determine if a referral to an oral surgeon is necessary.
Oral surgery procedures available at our Hamilton dental office
Financing Options & Direct Insurance Billing Available
Martindale Dental understands that oral surgery can involve costs that patients might be concerned about. That’s why we offer a choice of financing options, including flexible payment plans that ensure patients are able to get the treatments they need. We also take the burden of payment off our patient’s minds by offering direct insurance billing. This simplifies the payment process and reduces out-of-pocket expenses for patients. By accepting insurance payments directly, patients can avoid the hassle of filing claims or waiting for reimbursements. With these financing options and direct insurance billing, Martindale Dental aims to make dental care more affordable and accessible to all patients, without compromising on quality.
What to expect during your oral surgery procedure
If you’ve been referred to an oral surgeon, don’t panic. Even though it sounds serious, oral surgery is used for very common procedures all the time and is a large part of modern dentistry. Upon referral, you will meet with your oral surgeon for a consultation and examination. Your dentist or surgeon will be able to advise you about all aspects of your treatment, including pre and post treatment requirements, procedure process, recovery times and medical requirements. Oral surgery is typically done in a single appointment using local or general anaesthesia.
Initial consultation
Prior to your appointment you will have a consultation with the oral surgeon or your dentist. At this time, you will be told what the procedure entails, if sedation is required and what preparations you should make before your appointment. You will also be asked about your medical history and any medications you’re currently taking. You may also be informed about estimated recovery times and if follow up treatments are required.
You might need a ride
Depending on the type of sedation your oral surgery procedure requires, you might need to arrange for a pick up after your appointment. Most oral surgery is done as an outpatient procedure which means you will be discharged from the clinic shortly after your treatment. Ask a family member or friend if they can drop you off and pick you up because you may not be able to operate a motor vehicle safely until the anaesthetic wears off.
Eating, drinking & your oral surgery appointment
If your procedure requires general anaesthesia you will most likely not be allowed to eat or drink anything for 8 hours before your appointment. You will be made aware of any such requirements during your consultation prior to your surgery appointment. Local Anaesthetic do not require fasting, but you need to be careful eating and drinking after surgery as parts of your face will be numb and you could seriously injure yourself. If fasting is required, you will be advised to take an early morning appointment, so you don’t have to feel hungry all day.
After successful surgery you will be allowed to eat and drink at will, but soft foods only. In most cases, you will have a wound in your mouth that needs to heal, which can only happen if nothing disturbs it. Eating will be difficult for at least a few days as you’ll need to avoid biting and chewing anything (hard foods). We recommend researching a menu of shakes, soups, broths or pureed foods so you’ll have a few options to choose from as you recover. Do not sip anything through a straw because the suction created could cause complications such as persistent bleeding or dry socket. Avoid consuming alcohol for 24 hours after general anaesthesia.
Oral surgery and medications
You will be asked to provide all necessary information about your medical history to ensure there are no conflicts. Certain blood thinners can have a negative impact on recovery times and you might need to stop taking them up to weeks before surgery. You will be informed if any antibiotics are required and if you’ll need pain killers or other medications to aid your recovery. You might also be asked to begin taking certain antibiotics prior to your surgery appointment. It is recommended to pick up any required medications and painkillers before surgery, so they are ready when you need them.
Prepping your home for recovery
Once you are discharged from surgery you will most likely be in pain and tired. The last thing you’ll want (or even be able to do) is get your home ready for your recovery. This is something you really should take care of before your surgery.
• Clean up and organize your recovery space, such as your bedroom or the living room couch.
• Change the sheets to something you can clean easily or throw away.
• Keep multiple pillows at hand so you can keep your head and upper body elevated to reduce swelling and bleeding.
• Keep all your necessary items close at hand. These could include eyewear, Kleenex, drinks, TV remotes, books, magazines, cell phones, pain killers etc.
• Move your TV into your bedroom so you have something to keep you entertained.
• Prepare something to eat and drink so it’s handy when you need it during recovery.
• Stock up on ice packs or frozen peas so you have something to help reduce swelling and pain ready to go.
• Make arrangements to have a family member or friend stay with you for a few days after surgery to assist or have someone agree to be ready to help if you need them. This is especially important for elderly patients.
What to expect after oral surgery
You won’t know exactly how your body reacts to surgery until after it’s over. The majority of patients will make a full recovery and should notice a significant reduction in swelling and pain within a few days of surgery. In the meantime, you should be taking care of your symptoms, meaning using pain killers to stay comfortable and adhering to the directions for taking antibiotics or other prescribed medications. If you’re pain gets worse, bleeding persists, or you begin to feel sick, it is important that you contact our office immediately or visit an emergency care centre.
Tips for recovery after your procedure
After your surgery you need to be focusing on recovering as quickly as possible. You’ll likely be in pain and fatigued so getting some rest is important. Hopefully you’ve prepared your home, pre-made some food and picked up any medications you might need. Your pain will pass in a few days but until then you should do your best to relax and rest. Keep yourself comfortable and treat your symptoms with pain killers. Eating and drinking as soon as you feel able is also important to keep your body strong and focused on healing. Eat only soft foods and avoid sipping anything through a straw. Your head should be kept elevated, even while you sleep, to keep swelling down and discourage bleeding. You may consider rinsing your mouth with lukewarm salt water and carefully brushing your teeth as early as 24 hours after surgery. This will be your decision and you should only do so if you are confident you won’t disturb any open wounds or treatment areas.
Questions to ask your Hamilton oral surgeon
What is the planned surgery process?
How long will your surgery last?
What type of sedation will be required?
Will you require someone to pick you up after surgery?
Are you required to abstain from food or drink prior to surgery?
Which painkillers, antibiotics of other medications are required or recommended?
What is your expected recovery time?
Will follow up procedures or additional appointments be required?
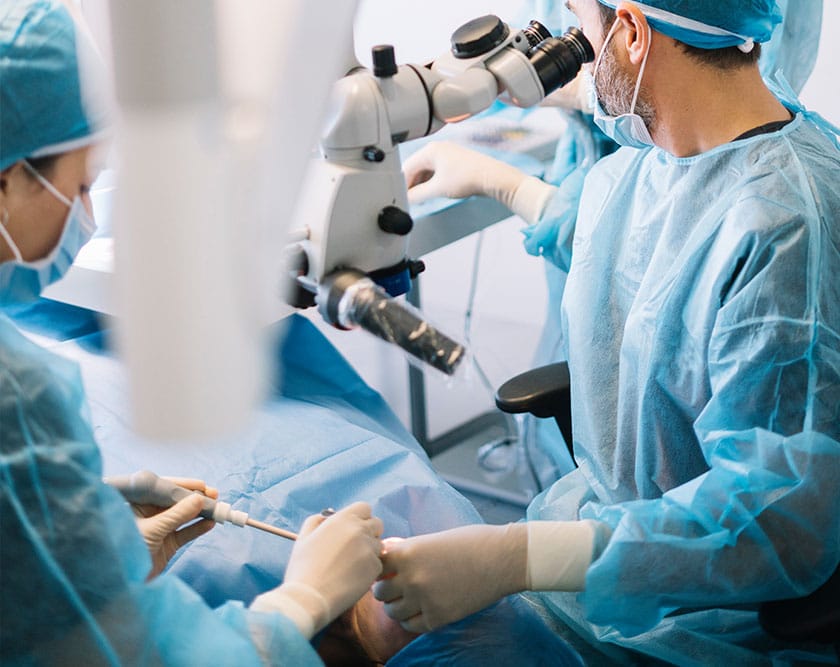

Questions to ask your Hamilton oral surgeon
What is the planned surgery process?
How long will your surgery last?
What type of sedation will be required?
Will you require someone to pick you up after surgery?
Are you required to abstain from food or drink prior to surgery?
Which painkillers, antibiotics of other medications are required or recommended?
What is your expected recovery time?
Will follow up procedures or additional appointments be required?
Please contact our office for more information:
Ready to restore
your smile?
Book your free consultation at our
Jackson Square Mall location now.
Please contact our office for more information:
Ready to restore
your smile?
Book your free consultation at our
Jackson Square Mall location now.
